- Free First Class Delivery
- Buyer Protection
- Secure Online Shopping
- Healthcare Professional? Click here
Arthritis


Categories
What is rheumatoid arthritis?
Rheumatoid arthritis is not just a joint disorder, it is a systemic autoimmune disease.
It is a disorder of the immune system whereby the body’s immune system attacks the patients joints leading to inflammation that results in joint damage and deformity. The onset of RA is not always linked with old age, however in the early stages it is possible to prevent the joints being destroyed completely.
Our everyday movements are a marvel of nature. Thanks to the complex interaction of joints, ligaments, tendons, and muscles, we are able to walk, dance and jump. If one of the over 140 joints is inflamed or irritated, the ingenious locomotor system becomes unbalanced. Such irritative conditions and inflammatory states of one or more joints are grouped together under the collective term "arthritis". Joint inflammation can start suddenly or take a chronic course. The most common chronic form of joint inflammation is rheumatoid arthritis.
Signs and symptoms
A classic feature of rheumatoid arthritis is the symmetrical onset of joint inflammation, whereby the joints of the fingers or toes on both sides of the body are affected at the same time. Inflammation of the joints becomes apparent through pain, swelling, warmth and mobility is restricted. Such inflammation usually begins in the joints of the fingers or in the joints of the hands and feet. It then spreads to other larger joints such as the knee and shoulder.
In many cases, fluid collects in the joint and causes swelling. Pain typically develops at rest. Whenever you move the joint, the pain eases.
In the early stages of the disease, this may be accompanied by secondary symptoms such as:
- Fatigue
- Exhaustion
- Loss of appetite
- Weight loss
- Raised temperature
Risk factors and causes
Rheumatoid arthritis is an autoimmune disease. This means that the body considers its own tissues to be foreign and fights them. The immune system reacts with an inflammation.
It is likely that a number of factors have to come together before rheumatoid arthritis can be triggered.
How can joint inflammation be treated?
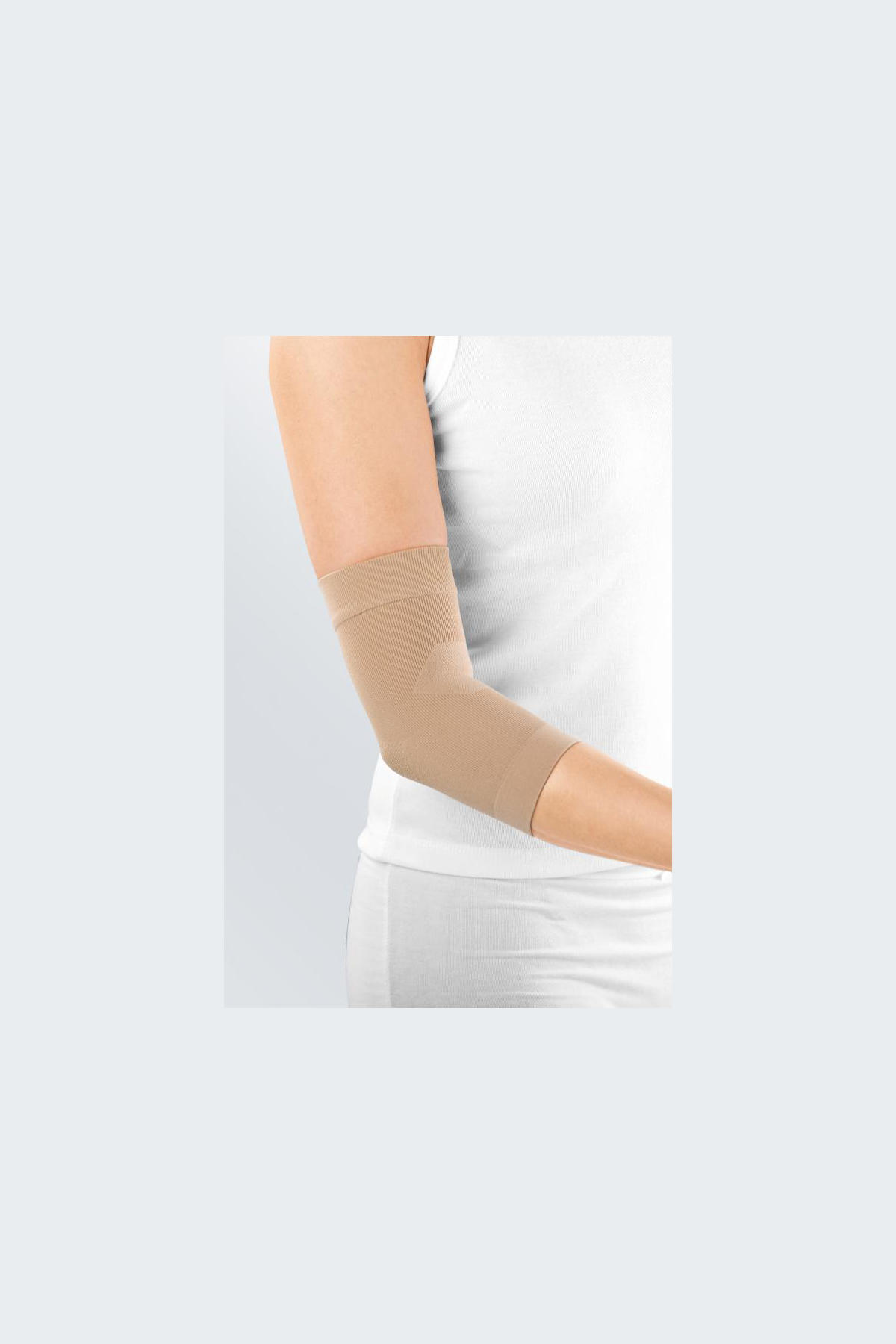
Medical supports have proved most valuable for rheumatoid arthritis. They stabilise and relieve the joint, reduce swelling and gently relieve pain.
There are other ways of stopping or reducing joint destruction apart from wearing supports. In the ideal case, an individual treatment plan is drawn up in collaboration between specialists, physiotherapists, occupational therapists and psychologists. Specialists in this field are, for example, rheumatologists, orthopaedic specialists and surgeons. Drugs are sometimes also prescribed for pain relief.
Other forms of treatment – also in combination with supports – are physiotherapy and exercises to do every day. Cold packs or special cold therapy can relieve pain. In some cases, an operation can help, e.g. the removal of the inner lining of the joint or replacement of the affected joint by an artificial one.
Talk to your doctor about which therapy is right for you.