- Free First Class Delivery
- Buyer Protection
- Secure Online Shopping
- Healthcare Professional? Click here
Venous leg ulcers (ulcus cruris venosum)


Categories
Venous leg ulcers (ulcus cruris venosum)
A leg ulcer/lower limb wound is defined as a break in the skin below the knee which has not healed within two weeks. These wounds can be painful, itchy and weep. There are various possible causes for lower limb wounds. About 1 percent of the western population is affected by an acute venous leg ulcer.*
Causes: How does a lower limb wound develop?
A lower limb wound can be caused by various conditions. The most common underlying condition contributing to leg ulceration is venous disease which accounts for 60-80 percent of all lower limb wounds.** The risk is likely to increase as people are living longer with multiple co-morbidities. Early accurate assessment will assist to diagnose the cause of the wound to ensure the patient receives the correct treatment. A classification tool identifies the different forms of lower limb wound according to the main circulatory disorder:
- Venous leg ulcer/wound: most severe form of chronic venous insufficiency (C6 according to CEAP, see below)
- Arterial leg ulcer/ wound: caused by arteriosclerosis / arterial calcification (PAD: peripheral arterial disease)
- Mixed aetiology leg ulcer/wound: with venous and arterial causes
- Other ulcers/wounds are as a result of other causes, such as pressure ulcers, or drug/treatment induced ulcers, malignancy, etc
Most common form: Venous lower limb wounds


60-80 percent of all lower limb wounds are regarded as venous-related.** Only around 10-30 percent are caused by arterial circulatory problems.***
10 – 20 percent suffer from a mixed aetiology wound caused by venous and arterial disease.***
The most common cause occurs due to severe chronic venous insufficiency. Over time a patient can develop venous valve incompetence (enabling blood flow to slip back down in the veins, rather than being propelled back towards the heart). This causes a build- up of pressure in the venous system causing enlarged veins, oedema and skin changes.
Signs and symptoms of venous disease
- C = Clinic (clinical findings)
- E = Aetiology (causes / trigger of the disorder)
- A = Anatomy (anatomical localisation)
- P = Pathophysiology (pathological dysfunction)
CEAP STAGES
| Stages | Changes |
| C 0 | No visible signs of venous disease |
| C 1 | Telangiectasias (spider veins) |
| C 2 | Varicosis (= varicose vein disorder) without clinical indication of a chronic venous insufficiency (= permanent vein weakness) |
| C 3 | Varicosis (= varicose vein disorder) with oedema (swelling) |
| C 4 | Varicosis (= varicose vein disorder) with trophic skin changes, subdivided into: |
| C 4a | Pigmentation (= skin changes) or eczema (= dermatitis, inflammatory skin reaction) |
| C 4b | Lipodermatosclerosis (= hardening of the subcutaneous fatty tissue) or atrophie blanche |
| C 5 | Varicosis (= varicose vein disorder) with healed ulcus cruris venosum (= leg ulcer, venous-related lower leg ulcer) |
| C 6 | Varicosis (= varicose vein disorder) with florid ulcus cruris venosum (= leg ulcer, venous-related lower leg ulcer) |
There are some physical skin changes which are a sign of venous disease and obtaining early treatment should reduce discomfort. This can be heavy, tired and itchy legs, and swollen, enlarged veins appearing on the legs and feet varicose veins. The venous blood is no longer being transported to the heart properly resulting in an increased pressure within the veins commonly referred to as venous hypertension. The increased volume of blood from the incompetent veins can lead to oedema, i.e. visible and palpable collections of fluid, forming in the tissue.
Skin changes of as an early stage of venous disease
Some skin changes could be an indicator that you are suffering with venous disease. Look for skin discolouration (brown-red discolouration caused by red blood cells being deposited in the skin), venous eczema (itchy, red, scaly, and/or flaky skin), lipodermatosclerosis (painful, hardened, tight skin), and atrophie blanche (star-shaped, ivory-white scars with surrounding skin discolouration). This stage can be described as pronounced vein weakness (medical term: chronic-venous insufficiency).
As a result of impaired venous return, the venous blood flows back into the capillaries: The smallest blood vessels that provide the cells with oxygen and nutrients are also responsible for the return transportation of metabolic by-products. The capillaries of patients who suffer from chronic venous insufficiency need assistance to support their faulty veins.
The smallest injuries can lead to a wound that does not heal
A minor injury, such as a knock from a car door or gardening injury, could lead to a break in the skin, resulting in a lower limb wound which may struggle to heal.
As a result of a wound patients may exercise less. This means that the calf muscle pump, which supports the vein system in transporting the blood in the direction of the heart, slows the venous return from already insufficient veins. A break in the skin can increase the risk of infection, which can further delay healing and cause unpleasant odours. A combination of pain, reduced mobility, odour and wound exudate can lead to patients becoming socially isolated.
Risk factors for lower limb wounds
The incidence of venous leg ulceration increases with age: From the age of 80, the frequency increases to around two percent.* As people age their activity can reduce, which results in the calf muscle pump not being stimulated regularly, causing blood to pool in the legs. Women are often more affected than men.* Other factors which increase the risk of skin problems are diabetes and smoking.
Genetic predisposition: Venous diseases are hereditary to some extent. It is likely that further members of your family may experience similar symptoms. Therefore, improved education around this topic can improve earlier intervention.
Pictures leg ulcer
Picture 1
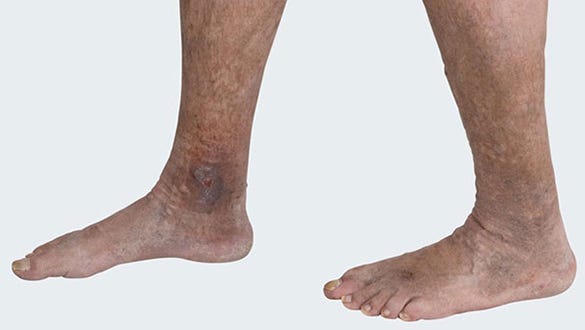

Picture 2
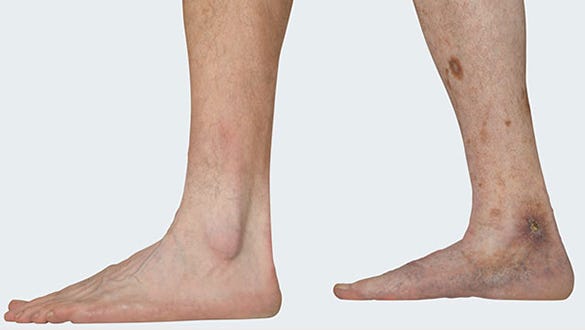

Picture 3
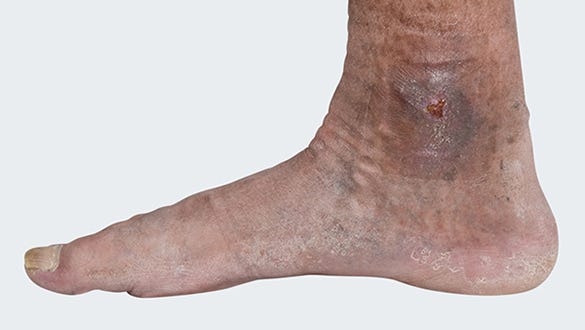

Picture 4
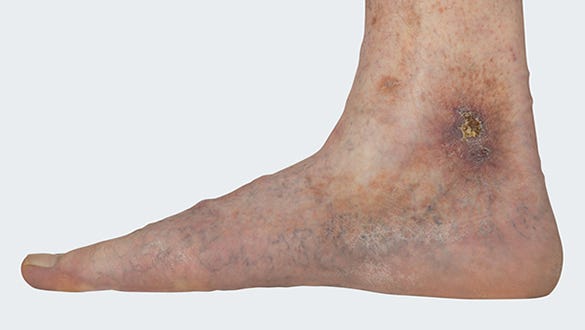

Preventing venous lower limb wounds: Top Tips options
Skin changes and a small wound on the lower limb can cause long term problems if not treated early. The best prevention is improving patient awareness, providing guidance on signs and symptoms to look for, and to get advice from a health care professional within the early stages so that the correct treatment can be started. If untreated venous disorders often do not cause a great deal of pain for patients for many years.
Treating venous lower limb wounds


When treating venous lower limb wounds, it is important to treat the underlying disease, i.e. the chronic venous insufficiency. The aim of the treatment is to improve the impaired return blood flow. The healthcare professional will discuss the treatment options available with the patient. Options may include wound cleansing, wound treatment with wound care dressings, compression therapy with medical compression stockings or adjustable, compression systems, as well as vein operations.
The medi therapy concept for the treatment of venous leg ulcer is based on international guidelines* ** **** as well as “medical compression therapy"*. Most importantly, medi products enable patients to participate within their treatment at each phase of their therapy.
Products from medi
Healing time: There are many factors that determine the healing process:
The duration of wound healing depends on various factors alongside the treatment that complies with the national guidance, such as the age of the patient, possible comorbidities and the location and size of the wound.
However, evidence indicates that although venous lower limb guidelines recommend compression therapy, over 80 percent of those with a venous lower limb wound do not receive compression therapy during the acute wound phase.***
After the ulcer has healed, the health care professional should carry out regular reviews to ensure that the wound does not return. This includes treatment with medical compression stockings.
Which health care professionals treat lower limb wounds?
Every patient with a lower limb wound should immediately seek medical treatment. Your first point of contact should be your Practice nurse. He/she will be able to guide you, whether specialist input is required for treating the lower limb wound:
- Specialist doctors, such Vascular Consultants, Dermatologists (skin specialists), Diabetologists (doctors who specialise in treating diabetes), are some of specialists who you may be referred too. They may hold clinics in hospitals or local medical practices.
- Certified wound advisers or Tissue viability nurses, are health care practitioners that may be contacted as required, as they have additional expertise in treating wounds. These specialists liaise with health care practitioners that may be treating patients with hard to heal wounds.
- Outpatient healthcare services are often an extension to GP services when caring for patients with chronic wounds. Some GPs have specially trained team members.
- Regional wound centres or outpatient clinics in hospitals employ expert teams to treat patients suffering from chronic wounds with dedication and experience.
Products by medi for the treatment of leg ulcers
Effective products, adapted to the individual phases of the therapy:
- Phase 1 - Wound debridement: UCS Debridement
- Phase 2 - Treatment for the underlying disease: circaid juxtacures, circaid juxtalite and mediven ulcer kit
- Phase 3 - Prevention of recurrence: mediven plus and mediven active
Phase 1 - Wound debridement


Only a clean wound will go onto heal
With UCS Debridement, a sterile cloth that has already been premoistened in a cleansing solution, the wound, wound edges and wound surrounding skin can be cleaned and moistened to achieve improved wound healing.
Phase 2 - Treatment for the underlying condition


Hence the lower limb wound is able to heal.
In the second phase of the therapy, medi offers an advantageous alternative for the therapy of venous leg ulcer with adjustable compression: circaid juxtacures.
- juxtalite can be easily adjusted and applied - the device can be easily applied and removed using Velcro straps. This can be very convenient if wound care dressings are required under the garment, access is easy and quick for patients and health care professionals.
- Controllable compression pressure is applied due to the integrated Built-In-Pressure system - the required compression pressure can be verifiably set and readjusted at any time.
- Once a wet, large wound has started to heal, it may be appropriate to use mediven ulcer kit . The two-component system consists of an easy to don understocking providing optimised hygiene and effective compression as well as a visually discreet, circular knitted outer compression stocking for additional compression during the mobile phase.
- With juxtalite also offers an alternative for those patients who have challenges with ulcer compression stockings (e.g. donning and doffing).
Phase 3 - Prevention of reccurence
To prevent recurrence of the leg ulcer
In venous lower limb wounds, the underlying disease, chronic venous insufficiency, persists even after the wound has healed. To prevent skin deteriorating in the future, long term treatment should be maintained with compression therapy. There are a wide variety of options to make this a fashionable and comfortable accessory, whatever your daily wardrobe.
For the time after wound healing, patients can choose from a wide range of medical compression stockings in a variety of colours and variations. Flat-knit compression stockings (e.g. mediven mondi ) are the ideal choice for patients with an additional disorder of the lymphatic system and consequently a tendency to lymphoedema.
If there is a venous swelling tendency, round knitted compression stockings (e.g. mediven plus) are used. This allows each patient to be treated individually in order to maintain the long-term success of the therapy.
For patients who have challenges with medical compression stockings (e.g. donning and doffing) adjustable compression devices (e.g. juxtalite) are an alternative to continue compression therapy.
Your Doctor or Clinician decides on your treatment therapy after diagnosing your condition. They will then prescribe the relevant wound care therapy products to meet the patient’s individual treatment plan.
* Harding K et al. Simplifying venous leg ulcer management. Consensus recommendations. Wounds International 2015.
** Scottish Intercollegiate Guidelines Network (SIGN). Management of chronic venous leg ulcers: a national clinical guideline. Edinburgh: NHS Quality Improvement Scotland; 2010. Available at www.sign.ac.uk/pdf/sign120.pdf (Last access 6 April 2020).
*** Sauer K et al. Barmer GEK Heil- und Hilfsmittelreport 2014. Available at www.barmer.de/presse/infothek/studien-und-reports/heil-und-hilfsmittelreport/report-2014-38588 (last access 6 April 2020).
**** O’Donnell T F et al. Management of venous leg ulcers: Clinical practice guidelines of the Society for Vascular Surgery® and the American Venous Forum. JVS, 2014;60(2):3S - 59S.
***** Rabe E et al. S2k-Leitlinie: Medizinische Kompressionstherapie der Extremitäten mit Medizinischem Kompressionsstrumpf (MKS), Phlebologischem Kompressionsverband (PKV) und Medizinischen adaptiven Kompressionssystemen (MAK). Available at: https://register.awmf.org/assets/guidelines/037-005l_S3k_Medizinische-Kompressionstherapie-MKS-PKV_2019-05.pdf (Last access 2 February 2024).