- Free First Class Delivery
- Buyer Protection
- Secure Online Shopping
- Healthcare Professional? Click here
Vein weakness: Venous insufficiency


Categories
Veins are the vessels in our circulation system that carry de-oxygenated blood away from our body tissues and back towards our heart. The Veins in our legs have an extremely hard job because they move the blood from the furthest distance at the very bottom of our legs, up against gravity. Because they work so hard, sometimes they become weak. When veins are weaker, they don’t work as well as they once did, this is known as venous insufficiency. A vein weakness left untreated can cause further problems to our lower legs such as varicose vein disorder (varicosis), swollen legs and ankles (venous oedema) and changes to the condition of the skin such as staining (hemosiderin). When weak Veins cause these symptoms, it is referred to as chronic venous insufficiency (CVI).
CVI causes – how chronic venous insufficiency develops


Veins usually work under high pressures every day. When we spend too much time standing still or seated the pressures in the leg veins can build. This happens also if we are immobile for long periods as the muscle pumps in our legs are not able to keep the circulation moving as it should when we move less. When the muscle pumps are not able to work as well, the veins expand to accommodate the increasing pressures. the diameter of the vessels increases as the veins expand further and further, and the venous valves responsible for stopping the back flow of blood no longer close effectively. The result of this increase in pressure in CVI, is often seen in the superficial veins under the skin becoming dilated from a build up of blood not effectively moving round in the venous circulation.
These dilated Vessels at the surface are best known as spider veins and dilation and twisting in the larger vessels caused by these increased pressures are called varicose veins. Left untreated these conditions can cause fluids meant for circulation by the Veins to leak out and into the surrounding tissues in the legs, causing swollen legs and ankles (Venous oedema).
Symptoms and signs of chronic venous insufficiency (CVI)
The symptoms of Chronic venous insufficiency may be any of the following symptoms below:
Varicosis


Veins that have become dilated due to CVI, measuring greater than three millimetres in diameter.
Varicosis with odema
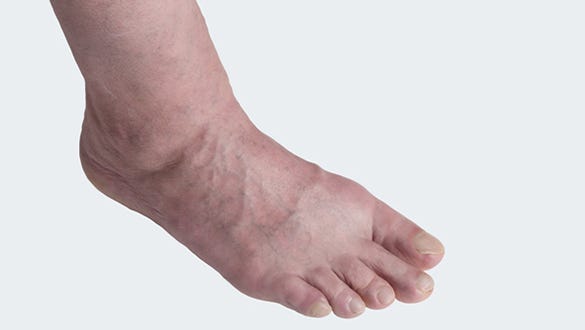

Swelling in the ankles and legs, this may appear gradually throughout the day and get better overnight with rest.
Skin changes
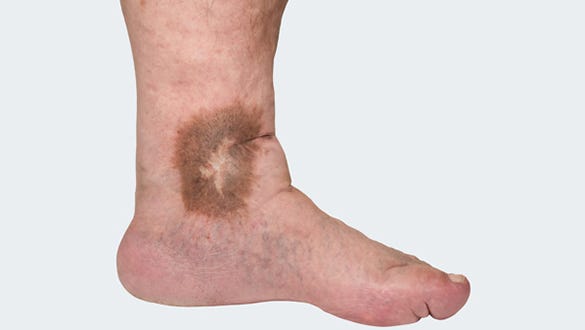

Brown or red discolouration or staining the skin (pigmentation), Changes to the condition of the skin such as dryness itching or Inflammation (varicose eczema), white atrophic scarring (Atrophie blanche), changed in the feel of the subcutaneous tissue becoming hard or woody (lipodermatosclerosis). *
Risk factors for developing CVI
Many people are at risk for developing CVI, some of the risks can be managed and reduced whereas others cannot. This makes awareness of the condition key to be able to implement prevention strategies. As we get older, the risk increases due to age-related loss of venous function, a hereditary predisposition is also noted therefore if members of your family have developed CVI you may be at a greater risk also. The influence of hormones on the body can also lead to a weakening of the venous wall, for example, during pregnancy. The risk factors for CVI are similar to those discussed in relation to varicose vein conditions.
Factors that can be influenced include:
- spending long periods of time sitting or standing (for example, at work),
- being overweight or obese.
- spending long periods of time in warm environments (for example, saunas, hot baths, underfloor heating)
- frequent consumption of alcohol
- Wearing tight clothing and high heel shoes.
Factors that cannot be influenced include:
- Age-related loss of function
- genetic predisposition
- hormonal changes that influence the veins, for example, during pregnancy.
The best way to keep your veins healthy is to live a balance and healthy lifestyle. Keep active and move as much as possible whilst maintaining a healthy diet.
Vein weakness prevention – tips for everyday life
Preventing venous insufficiency can be possible by making some simple yet effective lifestyle changes. By making positive changes to the the influenceable risk factors described above you can reduce your risks of developing poor vein health. Here are some everyday tips to help:


- Movement: Move as often as you can. This doesn’t mean you have to walk for miles simple changes to your position or frequently raising your legs when seated can help: It’s better to walk and lie down than to stand and sit.
- Sport and exercise: By being active you minimise the risk of high pressures building in your legs. See if you can add ten minutes of vein exercises into your everyday routine.
- Healthy diet: Try to eat a balanced and varied diet.
- Optimise your weight: Aim to keep your weight in range with national guidance and reduce any excess weight where possible.
- Clothing: Try to avoid tight fitting clothes and chose comfortable, loose clothing where possible.
- Shoes: Avoid long periods in high heels and where possible choose comfortable, well-fitting flat shoes.
Diagnosis and treatment of chronic venous insufficiency (CVI)
If you notice signs of chronic venous insufficiency, you should discuss this with your GP or Nurse. They may then decide to refer you to a specialist health care profession for a in depth leg assessment. This assessment can be completed by a wide range of medical professionals and who you are seen by will depend on your local clinical services available it may be a Tissue viability service, a vascular surgeon or a even a dermatologists). The healthcare professional will usually ask about your medical history, including current symptoms and any possible risk factors. This will be followed by a visual examination and physical palpitation. Throughout the examination, attention to skin changes and tissue will be made to identify any signs of CVI. Along with a clinical examination often further tests may be completed to look at the circulation in your lower limbs. This will often include looking to see if your Arteries are healthy (ABPI test) and tests to evaluate the level of any venous insufficiency based on an ultrasound image, such as an ultrasound examination (duplex sonography, Doppler sonography).
These are non-invasive examinations and should be quick, painless and are not associated with any risks!
Treatment of CVI using medical compression stockings
Once the veins are weakened and damaged there is no way to repair them. However, there are ways to help control further disease advancement and to significantly alleviate symptoms therefore improving quality of life. The first line treatment for the long-term management of CVI is the use of medical compression stockings along with plans to reduce your risk factors such as weight management or exercise activities. Medical compression stockings exert exterior pressure on the tissue and improve the action of the leg muscle pumps. If worn during movement, the muscles become tense, the veins between the muscles are compressed, and the compression helps the venous valves close better. As a result, improved circulation in the venous system from the legs back to the heart occurs. This improvement helps to alleviate symptoms such as pain, swelling and any tightness.
The most advanced and severe form of CVI – a leg ulcer (Venous ulceration) – In the management of venous leg ulcers compression therapy places a vital role in wound healing. Even once a leg ulcer has healed, the ongoing application of daily medical compression stockings ia recommended to prevent the development of further leg ulcers.* This is known as prevention of recurrence.
Besides the compression therapy, there are have been recent advancements in surgical interventions for treating vein insufficiency – surgical interventions are often minimally-invasive – procedures used to eliminate or remove the damaged/weakened veins. The best known are vein stripping, sclerotherapy and laser treatment. The general rule: You decide together with your doctor what measures are necessary and advisable. You can find further therapy measures here.
Compression stockings by medi
What happens if the venous insufficiency is not treated?
Venous insufficiency is progressive and can be the term used to describe a wide range of symptoms. If let untreated symptom can become more serious overtime and can have an increasing affect on daily activities and quality of life.This includes the following:
- Further Skin colour changes (Hemosiderin)
- Varicose Eczema (inflammatory skin diseases)
- Cellulitis (a bacterial infection of the deeper layers of the skin)
- Leg ulcer (venous leg ulcer)
- Chronic Oedema (swelling in the leg that does not reduces with elevation)
Your Doctor or Clinician decides on your treatment therapy after diagnosing your condition. They will then prescribe the relevant wound care therapy products to meet the patient’s individual treatment plan.
* Rabe E et al. Indications for medical compression stockings in venous and lymphatic disorders: An evidence-based consensus statement. Phlebology 2018;33(3):163-184.