- Free First Class Delivery
- Buyer Protection
- Secure Online Shopping
- Healthcare Professional? Click here
Osteoarthritis of the knee


Categories
What is osteoarthritis?
Osteoarthritis is the most common form of arthritis. It is a slowly progressive inflammatory degenerative disease of the knee joint. It occurs when the cartilage that acts as a cushion at the end of your bones, breaks down and wears over time. Pain radiates from the joint structure and is usually felt when bending the knee, when climbing stairs and after long periods sitting or lying down. Morning pain from stiff joints is a common complaint in the early stages of knee joint osteoarthritis. This pain usually subsides after the joint has been active for a while. The disorder most commonly affects joints in the hands, knees, hips and spine. A worn joint can become inflamed. This then becomes activated osteoarthritis with inflammatory phases. Medication aims to keep the inflammatory phases as brief as possible.
Types of knee osteoarthritis
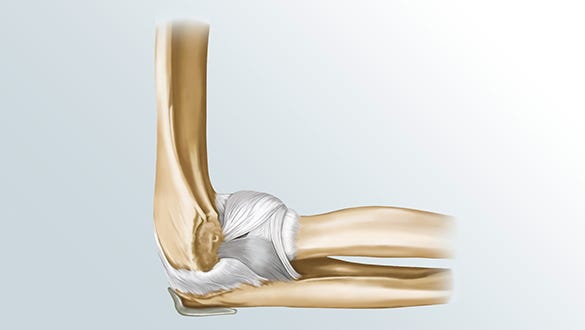
Three bones come together to make up the knee joint:
- The thigh bone (femur)
- The kneecap (patella)
- The shinbone (tibia)
Joint wear and tear is when the bone surfaces rub together. The joint between the thigh bone and the shinbone consists of two joint sections: the inner (medial) and outer (lateral) parts.
- Medial knee osteoarthritis is when the inner section of the knee joint is affected by wear and tear, this is medial osteoarthritis.
- Lateral knee osteoarthritis is when knee osteoarthritis is in the outer area of the knee, this is referred to as lateral osteoarthritis.
Causes of knee osteoarthritis
There is often no clear or concrete cause for knee joint arthrosis. In most cases, it is “primary osteoarthritis” – caused by age-related wear and tear of the cartilage. Other cause can be congenital misalignments (bow-legged or knocked-kneed) and illnesses or injuries can result in joint wear and tear. These are referred to as “secondary osteoarthritis”.
Symptoms and signs of knee osteoarthritis
Symptoms often develop slowly and worsen over time. Signs and symptoms often include:
- Pain - affected joints might hurt during or after movement.
- Stiffness - joint stiffness might be most noticeable upon awakening or after being inactive.
- Tenderness - your joint might feel tender when you apply light pressure to or near it.
- Loss of flexibility - you might not be able to move your joint through its full range of motion.
- Grating sensation - you might feel a grating sensation when you use the joint, and you might hear popping or crackling.
- Bone spurs - these extra bits of bone, which feel like hard lumps, can form around the affected joint.
- Swelling - this might be caused by soft tissue inflammation around the joint.
Osteoarthritis stages: grades of joint wear and tear
There are four grades of severity for knee osteoarthritis, depending on the degree of wear and tear.
Osteoarthritis Grade I
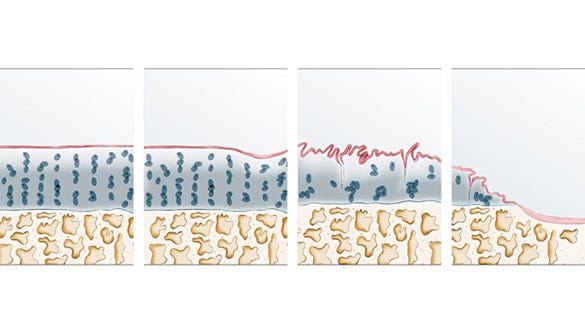

The cartilage layer in the knee has become very soft but is still undamaged. The stage is largely symptom-free, and the function of the joint is not yet impaired.
Osteoarthritis Grade II
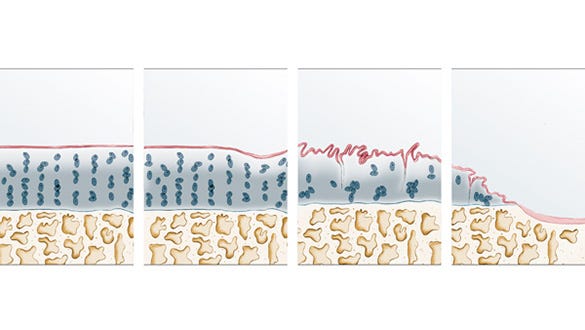

The first damage to the cartilaginous cell structure may have occurred and the cartilage surface appears roughened up. Again, as with Grade I, there are usually no symptoms at this stage or functional impairments of the knee joint.
Osteoarthritis Grade III


The cartilage surfaces are damaged. The first cracks form. The person suffers from joint pain as the cartilage layer has worn away in places.
Osteoarthritis Grade IV
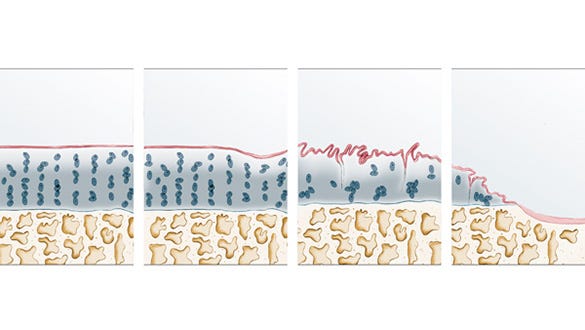

Total cartilage loss causing the exposed bone surfaces rub against each other. This is known by experts as Chondromalacia grade 4. Abrasion in the knee joint causes stiffening and painful inflammation, swelling and joint effusion.
Risk factors for osteoarthritis
Accidents during sports and in your leisure time
Knee injuries, particularly of the menisci and ligaments, can cause natural wear to start earlier or speed up the degeneration process. The rupture of the anterior cruciate ligament (ACL) is one of the most common knee injuries. A consequence of this injury is often instability of the knee joint, which in the long term can lead to increased wear of the cartilage (cartilage degeneration) – and thus to the development of osteoarthritis**. Even injuries that occurred many years ago and seemingly healed, can increase your risk of osteoarthritis.
Lack of exercise
Exercise is essential for the nutrition of the cartilage. As the cartilaginous layers are not supplied with blood, metabolic products and nutrients can only be absorbed by movement.
Genetic predisposition
Exercise is essential for the nutrition of the cartilage. As the cartilaginous layers are not supplied with blood, metabolic products and nutrients can only be absorbed by movement.
Being overweight
Carrying extra body weight contributes to osteoarthritis in several ways. The more you weigh, the greater your risk. This increased weight puts additional stress to weight-bearing joints, such as your hips and knees. Another factor is that fat tissue produces proteins that can cause harmful inflammation in and around your joints.
Sex
Women are more likely to develop osteoarthritis, although it isn’t clear why.
Repeated stress on the joint
If your job or your sport places repetitive stress on a particular joint, then that joint may develop osteoarthritis due to wear and tear.
Certain metabolic disorders
Changes to the cartilage metabolism also worsen nutrient supply to the cartilage. These include diabetes and hemochromatosis (a condition which your body has too much iron.
How can I prevent osteoarthritis?
Years of being overweight can cause additional stress on joints thus significantly increasing your chances of developing osteoarthritis due to wear and tear. If you have a BMI (body mass index) of over 25, you are classed as overweight. A BMI of over 30 is classified as being severely overweight or obese. People with osteoarthritis are therefore often advised to lose weight by their clinicians.
Self-management – how to improve your quality of life
Osteoarthritis sufferers can do a certainly help themselves to reduce pain and improve treatment outcomes by being more active in dealing with the disease. For example, eat a healthy diet, losing weight and taking regular physical, but gentle, activity.




Nutrition for osteoarthritis
Nutrition plays a significant role in the development of arthrosis. Nutritional changes cannot cure arthrosis but can have beneficial effects.
Pay attention to your diet and weight: Study on weight and osteoarthritis
A recent Australian study examined the connection between being overweight and developing osteoarthritis of the knee. Patients of a healthy weight only developed osteoarthritis at an older age, while young, healthy but overweight patients saw a decrease in the cartilage at a younger age.*
Sport and exercise with osteoarthritis
One thing we know for sure is that sport and exercise are invaluable both for those already with osteoarthritis and those looking to prevent it! When in pain, people often prefer to rest and try to move the knee as little as possible. This is definitely the wrong thing to do. Lack of exercise is one of the main risk factors for arthrosis.
Targeted training of the arthritic joints strengthens the muscles and improves coordination and balance. Movement produces more synovial fluid, which leads to less abrasion and more flexible joints.
Which sports are suitable for those with osteoarthritis?
Examples of beneficial sports with gentle movements
- Swimming
- Aqua aerobics
- Cycling
- Golf
- Walking
Examples of unsuitable “contact” sports
- Football
- Skiing
- Tennis
- Basketball
Find the sport that you enjoy. Avoid sports-related strain. If you are unsure of whether you can do a specific sport, ask your physio for advice.
Therapeutic measures – what helps in osteoarthritis?
Although osteoarthritis is incurable, numerous treatment options can relieve pain and make everyday life easier.
Conservative therapy
Non-pharmacological therapy
- Orthopaedic aids (such as insoles, supports, braces)
- Physiotherapy
- Physical therapy (e.g. magnetic field therapy, ultrasound, electrical stimulation, shockwave)
- Occupational therapy
- Naturopathy (e.g. acupuncture, aqua aerobics)
Pharmacological therapy
- Medication (painkillers, anti-inflammatory drugs)
Six home exercises
Exercises that can be performed without pain can counteract the progression of the osteoarthritis. The examples listed here are not just beneficial for the knee - they support your entire body.
Surgical measures
Joint preservation
Arthroscopy
A rarely used therapy for knee osteoarthritis is arthroscopy, in which a small camera (endoscope) is inserted into the knee joint to obtain a clear picture of the interior of the joint and to decide on suitable therapy measures.
Osteotomy
In osteotomy, a wedge of bone is removed or inserted to correct misalignments or arthrotic damage on one side of the knee joint. By correcting the leg axis, the affected cartilage is relieved, thus preventing increased wear.
Joint replacement
Partial joint replacement
If only one side of the knee joint is affected by osteoarthritis, there is the possibility of surgery. In a partial joint replacement surgery, only the destroyed or affected side of the knee joint is replaced with metallic or plastic components. This operation is also known as an unicompartmental knee joint replacement. The healthy side is preserved.
Complete joint replacement (full knee prosthesis)
This operation is only considered if both sides of the knee surface have been significantly destroyed and the patient is in so much pain that they cannot be helped by other therapies. During the operation, the destroyed surface of the knee joint is replaced by metallic and plastic components. These are shaped to best match the anatomy of the knee joint.
More information
*Arthrose. Gesundheitsberichterstattung des Bundes; Heft 54. Herausgeber: Robert Koch-Institut, Berlin 2013. Published online at: www.rki.de/DE/Content/Gesundheitsmonitoring/Gesundheitsberichterstattung/GBEDownloadsT/arthrose.pdf (Last accessed: 27.02.2018).
**Paschos NK. Anterior cruciate ligament reconstruction and knee osteoarthritis. World J Orthop. 2017;8(3):212–217.