- Free First Class Delivery
- Buyer Protection
- Secure Online Shopping
- Healthcare Professional? Click here
Lymphoedema


Categories
What is a lymphoedema?
Our lymphatic system is connected to our cardiovascular system and fulfils functions for our organism that are just as important as the cardiovascular system itself. It plays a decisive role as part of our immune system. As long as we are healthy, there are hardly any reasons for thinking about the lymphatic system. We only become aware of it when it is impaired – in the case of lymphoedema, for example.
Lymphoedema occurs if the lymphatic system is damaged. Lymph vessels form part of your circulatory system which helps fluid to move around your body. If fluid is unable to effectively drain, lymph fluid builds up in the spaces of the body tissue which causes swelling. If left untreated the swelling will get worse and the condition becomes chronic, but with the right treatment, those affected can achieve very good outcomes. Lymphoedema mainly occurs in the arms or legs.
However, with the right treatment, it is possible to lead an everyday life that is as normal as possible. Because one thing is for sure: there are ways of keeping lymphoedema constant and enjoying life all the same.
The body's "hazardous waste disposal" service
The lymphatic system can be compared with “hazardous waste disposal”, because it transports waste products out of the body. These include, for example, proteins, metabolic breakdown products, inflammatory products or fat from the abdominal cavity. The lymphatic system runs alongside the blood vessels and covers our entire body like a net.
Every day it transports up to four litres of purified lymph back into the blood circulation. Lymphoedema can develop if lymphatic drainage is interrupted or impaired. There are so many different treatment options available today that you can lead an almost perfectly normal life, even with lymphoedema.
Types of Lymphoedema
Lymphoedema may be caused by a congenital problem (primary lymphoedema) or occur at a later stage of life (secondary lymphoedema).
Primary lymphoedema
This type of lymphoedema is caused by a genetic fault. In most cases, lymph vessels or lymph nodes were not properly formed. The symptoms of primary lymphoedema can appear immediately after birth, but usually appear at a later stage in life.
Causes of primary lymphoedema:
- complete absence of lymphatic vessels
- lymphatic vessels are too narrow or are missing
- expanded vascular walls
- hardening of the lymph nodes
- absence of lymph nodes
Primary lymphoedema may also be a component in syndromes such as Klippel-Trénaunay syndrome.
Resulting from external influences: secondary lymphoedema
This form of lymphoedema refers to oedema that only occurs during life and is not congenital. Secondary lymphoedema results from external influences:
- operations/ surgery (lymph nodes completely or partially removed)
- radiotherapy
- malignant diseases, such as tumours
- injuries
- skin inflammation (e.g. erysipelas)
- untreated venous disease
- obesity
Lymphoedema: Symptoms and signs
It is advisable to seek help if you develop any symptoms of lymphoedema. The following signs may indicate lymphoedema:
- swelling in one limb only (unilateral)
- jewellery and clothing become tight
- natural skin folds become deeper
- gradual hardening of the skin
- positive Stemmer’s test (unable to pinch a fold of skin)
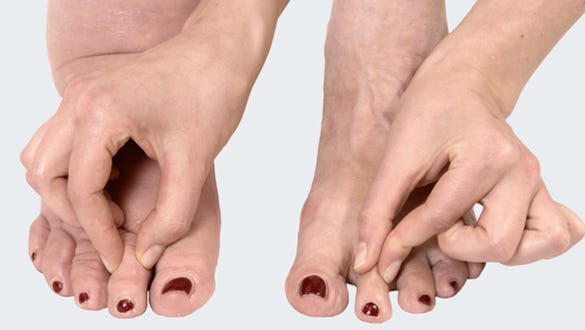
Recognising lymphoedema with Stemmer’s test
The ‘Stemmer's sign’ is a reliable way of detecting lymphoedema.
- positive Stemmer’s sign: Try to lift a fold of skin at the base of your toes, if this is hard or impossible, this is a ‘positive Stemmer’s sign’. This is a sign of lymphoedema.
- negative Stemmer’s sign: if it is easy to lift a skin fold, this is called a negative Stemmer's sign. This indicates that no lymphoedema is present, but it does not fundamentally rule out lymphoedema. Please seek advice from a nurse or doctor.
Your nurse or doctor should start appropriate treatment or refer you to a specialist practitioner. The earlier treatment starts, the more likely it is to keep the oedema under control in the long term.
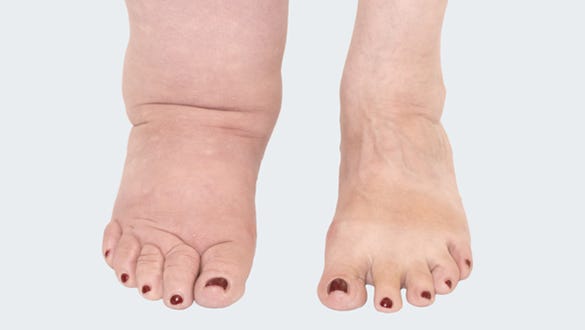


Stage 0
Latent lymphoedema
- the lymph vessels are damaged, but no swelling is visible yet, lymph drainage is normal
- no oedema exists (yet)
Stage 1
Oedema which resolves after limb elevation
Swelling occurs during the day, which reduces or resolves when the area of swelling is elevated. When pressure is applied to the tissue, a dent is formed which remains for some time. This is known as pitting oedema
- impaired lymph drainage
- oedema occurs during the day
- reduction of the oedema after lying down with the affected area elevated such as overnight, when in bed
- visible dent after strongly pressing with the finger


Stage 2
Oedema which is not resolved by limb elevation
The swelling remains even during longer rest periods. The skin is hardened and elevating the arms or legs does not bring any relief or resolve. Pitting oedema is not present.
- no reduction of the oedema after limb elevation (going to bed)difficult
- or impossible to press the skin indentation inwards (non-pitting oedema)
- skin changes occur – the texture of the skin becomes uneven and soft ‘bobbles’ appear which may leak lymph fluid
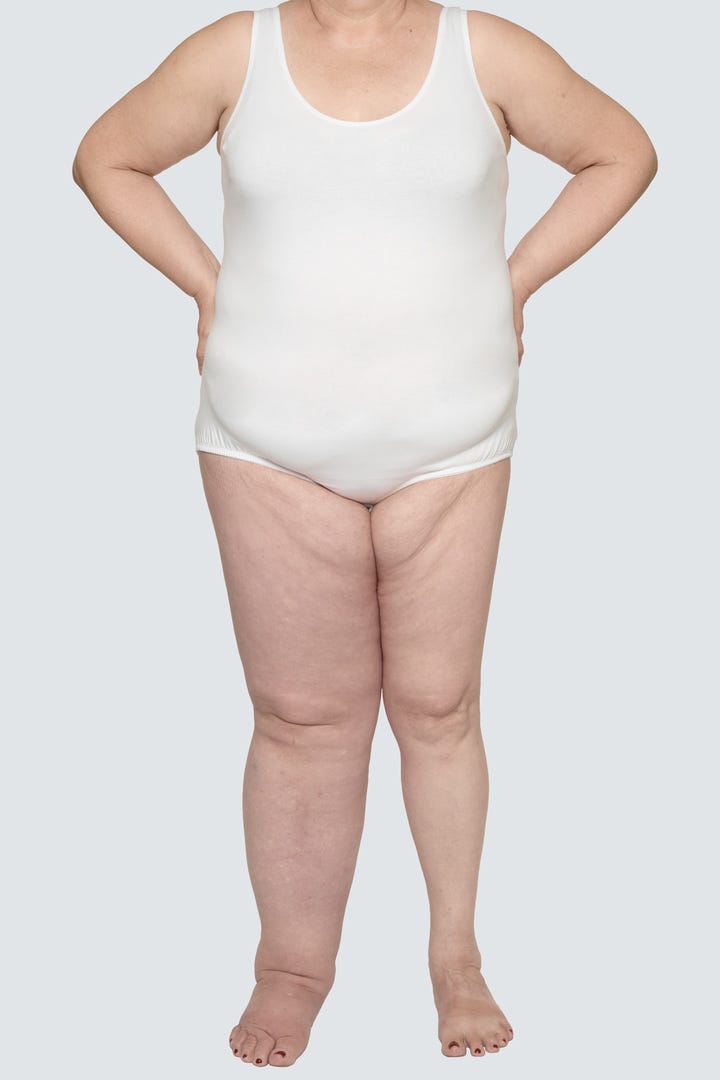

Stage 3
Elephantiasis
If the swelling remains untreated the limb shape becomes distorted exaggerating the skin folds. The skin condition will continue to get worse and the ‘bobbles’ become hardened and lymph fluid will continue to leak. This stage is often called ‘elephantiasis’.
- The shape of the limbs becomes distorted
- hardened skin
- wart-like growths from which lymph can trickle
- complications: skin infections (erysipelas, cellulitis), deep wounds which do not easily heal
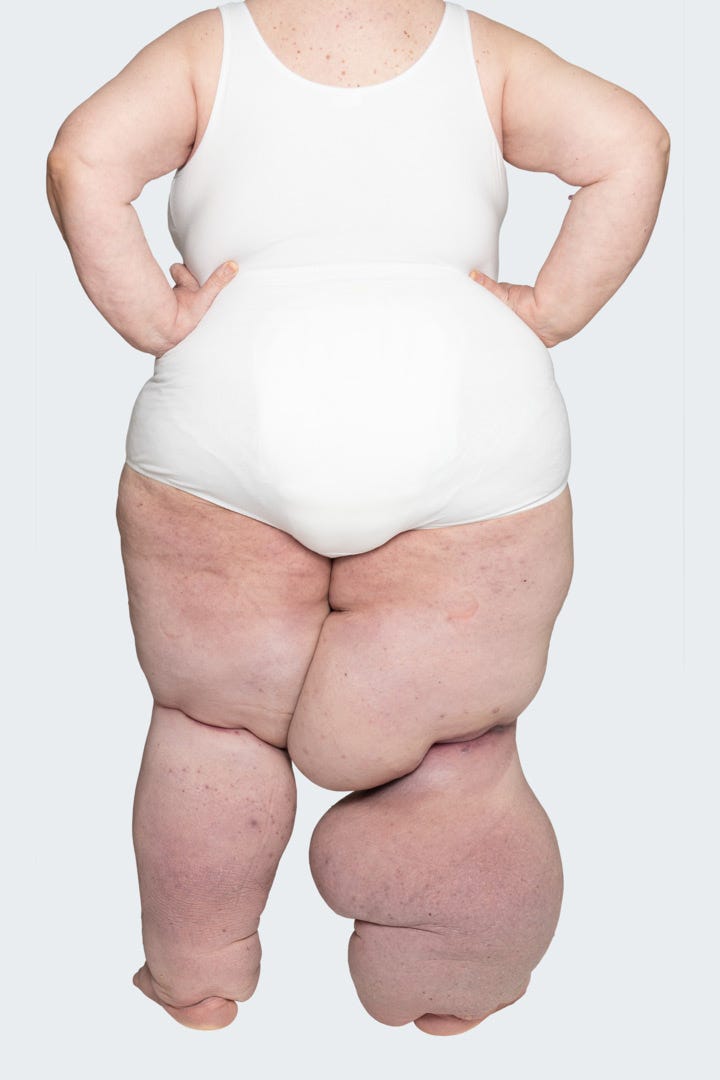

But in all cases, it is advisable to consult a doctor at an early stage (already at stage one). He can recommend suitable treatment and make sure that the oedema does not develop further, but is reduced or at least stays constant. This way you can prevent oedema progressing to stage 3.
Lymphoedema after surgery for breast cancer
Breast cancer is the most common form of cancer in women. Over 70,000 new cases are diagnosed every year.*
On average, 20 to 30% of patients are affected by breast cancer-related lymphoedema following removal of the axillary lymph nodes and adjuvant radiotherapy.**
Lipoedema and lymphoedema
Lipoedema is a disorder caused by an abnormal fat distribution of the subcutaneous tissue on the legs and arms. If the subcutaneous fatty tissue exerts considerable pressure on the lymphatic channels, secondary lymphoedema may occur.
Lymphoedema and venous disease
Damage to the veins (chronic venous insufficiency) can also be the cause of secondary lymphoedema. With chronic venous insufficiency, there is increased fluid leakage into the tissue. Initially, the lymphatic system removes this increased amount of fluid. If the lymphatic system is permanently overloaded, it can lose its function resulting in protein-rich oedema.
Risk factors
Patients with cancer often have to have radiotherapy of their lymph nodes or the nodes are removed altogether. Naturally, this influences the whole lymphatic system, so oedema can develop. Other factors such as age or simply the fact that one is a woman can favour the onset of lymphoedema.
In many cases, lymphoedema also develops from a previous venous disorder combined with too little physical exercise. There are many causes, but the good news at this point is: there are efficient treatment options available to give lymph patients their quality of life back.
Prevention
Do you have lymphoedema? Pay attention to the small things in everyday life. These will all make a contribution to keeping your oedema in check. For instance, wear comfortable clothes that do not constrict you. Clean and care for your skin carefully and only use pH neutral substances. At home, protect yourself against injuries to your nails and skin. Avoid stress and extreme cold, because both of these constrict the vessels. Activities that dilate the vessels such as sunbathing for a long time, visiting the sauna or having a hot bath are not recommended either. Also important: while manual lymphatic drainage has a positive effect on the lymph system, you should avoid kneading massages. These could over-stress the affected part of your body. And last but not least: wear compression garments whenever you exercise.
Living with Lymphoedema – Education, Therapy, Quality of Life
Lymphoedema changes lives. For the patient the chronic disease is a constant companion in all aspects of life. But what is the best way of dealing with the disease symptoms? Which therapy is suitable? How can I live a normal life despite lymphoedema? The film “Living with Lymphoedema – Education, Therapy, Quality of Life“ from medi gives concrete answers as well as practical tips for everyday life.
How can lymphoedema be treated?
Lymphoedema is a chronic disease. However, long-term treatment does achieve very good results. Complex physical decongestion therapy (CPD) has proved particularly successful. The therapy consists of two phases and five stages. The aim is to first decongest the affected limbs – as the name suggests.
Initially the focus is on skincare and hygiene. Clean and care for the affected areas. The therapist then performs manual lymphatic drainage before applying a compression bandage immediately afterwards. This encourages the return flow of lymph fluid during this phase. Without the bandages, the oedema would return after about two hours. As part of the decongestion process, it is important to move around – preferably directly after the manual lymphatic drainage and with the bandaging in place.
Once the decongestion phase is complete, the second phase will start: the maintenance phase. The four components are the same as in decongestion: hygiene, lymphatic drainage, compression and physical activity. But now the compression dressing is replaced with a compression garment. Flat knit compression stockings are usually used for this. These are seamed garments that are made of less elastic, stiffer material than round knit garments. Round knit hosiery is used more for venous diseases such as varicose veins.
The two phases of treatment
Not all phases are performed or needed and your specialist will determine what is best for you.
Phase 1 - Decongestion phase
The aim is to reduce the circumference of the affected limbs. So in the first phase of complex physical decongestion therapy (CPD), manual whole-body lymphatic drainage is performed once or twice a day to promote the return transport of the fluid away from the tissues. A compression dressing is applied after each treatment session. The decongestion therapy is also supported by special exercises. When beginning treatment, skin conditions such as fissures or athlete's foot are treated intensively, because an inflammation can cause additional damage. Consistent skin hygiene and care are also important later on. Only pH-neutral cleaning products and creams may be used.
The first phase of complex physical decongestion therapy lasts about three to six weeks. The individual duration depends on how successful decongestion is. Once the circumference of the affected regions of the body can no longer be reduced any further, we then go on to the maintenance phase.
Phase 2 - Maintenance phase
The aim of phase 2 of complex physical decongestion therapy (CPD) is to maintain the successes and results gained in phase 1. During this treatment phase, manual lymphatic drainage should be given at least once a week in winter and twice a week in summer. Compression therapy is still supported by compression garments/sleeves/hand parts and toecaps. The additional treatment measures such as special skin care and exercises must not be neglected either during this phase.
The five stages of treatment (also called DLT: Decongestive Lymphatic Therapy)
Hygiene& skin care
Daily thorough skin care is essential for lymphatic conditions: the skin is particularly sensitive and tends to become dry and itchy. Infections, inflammations, and wound healing disorders may develop quickly, because the upper layer of the skin is often not supplied with sufficient moisture and the skin can no longer perform its natural barrier function. The medi care series may only be used on undamaged skin and is tailored to the needs of compression stocking wearers.
Tip: With lymphoedema therapy, even minor skin irritations should be taken seriously. Always report skin changes to your practitioner.


Compression therapy
In the decongestive phase, compression therapy is applied after each MLD session. This is adjusted to the daily changing circumferences of the affected limbs. Without compression, the affected area would quickly swell again.
In the maintenance phase, medical compression hosiery is applied to prevent the recurrence of oedema. This is prescribed by your lymphoedema specialist, nurse or doctor and many styles are available on GP prescription.


Exercise& movement
Exercise and movement are important to maintain circulation and lymph flow. It is especially important to move straight after manual lymphatic drainage and with compression being worn. Movement and compression therapy are beneficial to each other, the movement of the muscle pump helps compression to work effectively and move fluid out of the area of congestion.


Manual lymph drainage
Manual lymph drainage (MLD) is a massage technique performed by specialist therapists: a lymph therapist stimulates lymphatic drainage with certain movements. This stimulates the lymphatic vessels to work harder, i.e. to better remove lymph fluid from the tissue.


Learning& self-management
To get the best results from the treatment try to keep motivated and as independent and active as possible under the guidance of a therapist. There are many self-help leaflets and educational material that can help understanding of this condition.
Infographic nutrition for lipoedema and lymphoedema
Discover how the right nutrition can contribute to greater wellbeing.


Who treats lymphoedema?
Your GP may be able to treat you straight away or may refer you to a lymphoedema specialist practitioner. There are lymphoedema clinics in many areas of the UK. Your practitioner may prescribe treatment (for example medical compression stockings) if necessary.
Lymphoedema network groups combine therapy knowledge and practice
Lymphoedema network groups exist in many regions. They are a group of people with many skills who work to improve many aspects of care for those with lymphoedema, lipoedema and venous disease.
They provide the most up to date educational information to guide and support affected people.
Lymphoedema networks maintain a constant exchange of experience, they continue to learn from each other and hold educational events for those affected. The purpose of such collaborations is to guarantee a high level of diagnostic and therapeutic reliability through close cooperation – with the aim of achieving optimal treatment results and an improved quality of life for patients.
Research a lymph network in your area online.
Flat knit compression garments for maintenance
Flat knit compression garments exert constant pressure on the arm or leg during the maintenance phase. They do not crease into skin folds, which could lead to constriction. Compression hosiery is available on prescription from medical retailers (e.g. surgical appliance retailer) and is made to measure to suit the circumference of the arm or leg.
The measurements are also taken by the surgical appliance retailer. It is important that you wear the garment regularly. Only then will the result remain constant and the oedema does not spread. Medicines can be taken as add-ons to treat oedema – your doctor will decide whether these are needed.
In summary, it can be said that lymphoedema is not entirely curable. However, very good results are achieved with CPD. Compression garments these days are even available in fashionable colours and patterns, so patients are far happier to wear them than ever before.