- Free First Class Delivery
- Buyer Protection
- Secure Online Shopping
- Healthcare Professional? Click here
I have a swollen leg


Categories
Water retention in the legs
Fluid build up under the skin, commonly starting at the foot or ankle is known as oedema. If you suffer from heavy legs and swollen ankles there could be a variety of reasons which should always be diagnosed by a GP/Doctor so you can be pointed towards the most appropriate therapy.
Water in the legs: risk factors and causes
The most frequent cause of fluid build-up in the legs is due to a weakness in the veins. Conditions with other organs in the body or metabolic disorders can also cause swelling to occur.
Venous oedema
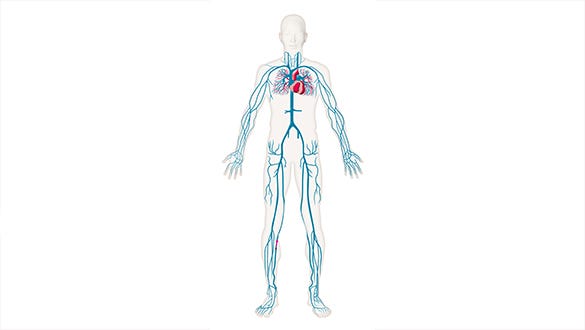
Venous disease can be a cause of swelling. In Venous disease, the blood is not able to return easily back to the heart due to poor functioning venous valves, and the pressure builds up in the veins and leaks fluid out from the smallest blood vessels (the capillaries) into the tissue. Therefore, the water build-up is known as venous oedema. The swelling usually begins in the ankles as this is where the highest pressure is.
Swollen legs
If both legs are suddenly swelling in the day, but reducing at night once you are in bed, this could be a symptom of heart failure.
Lymphoedema
In lymphoedema – often the swelling occurs to one limb only – this indicates that the lymph nodes in that area are not functioning correctly and are unable to filter the fluid from the leg back into the rest of the body.
Metabolic disorders
People who experience kidney, liver or thyroid disease often suffer with swollen legs. This is because imbalances of protein, fluid and minerals in a metabolic disorder influences how fluids are dealt with in the body.
Further possible causes to swollen ankles could be allergies, medicines hormone disorders etc. therefore it is vitally important to check with your GP to establish the cause and appropriate treatment.
Why do weak veins cause swollen legs?
The calf muscle is has an important function in helping return blood back up to the heart, therefore when we sit of stand for long periods, the pressure in the ankles increase, and it is only when we move our ankles that the calf muscle can work. In the example of standing for a long period, the blood pools, the pressure increases, (known as venous hypertension) and the vessels leak fluid into the tissue. This results in ankle swelling – especially noticeable by the end of the day.
Swollen legs during pregnancy
Leg swelling can occur during pregnancy. Due to the increased amount of blood in the body and also due to the weight of the abdomen pressing on the veins in the thigh and causing a back pressure.
Products by medi that support you during pregnancy
What helps with water retention in the legs?
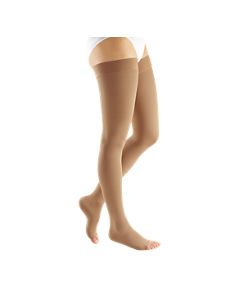
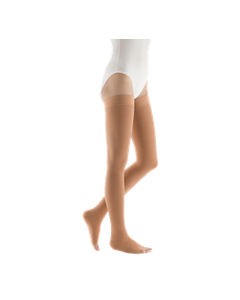
Basic therapy: medical compression stockings
The simplest therapy available for venous disorders is to wear medical compression stockings. Many studies show that venous oedema can be treated very effectively with medical compression swelling is reduced when wearing them and continual wearing during the daytime prevents the oedema reforming.*
Compression is particularly effective when combined with movement and exercise. During movement, the muscle pump activates, and venous valves are more efficient at closing and therefore pushing the blood back up to the heart.
Medical compression can also help relieve the other symptoms associated with venous disorders such as heaviness, tightness, pain as well as swelling and improve quality of life.
Find out about vein therapy here.
Which doctors treat water retention in the legs?
Your GP would want to know about medical history including symptoms and any comorbidities (other conditions you have).
They can then asses the limb and condition of the skin, and underlying oedema, by inspecting and touching it to see how much oedema is present.
A Vascular Surgeon is able to visualise the blood flow by using ultrasound or scanners (duplex scans etc) these investigations help to establish whether the cause of the problem is superficial (surface veins) or a problem in the deep venous system.
medi compression stockings


Due to the breathable, stretchy material medical compression are very comfortable for men or women to wear and are adapted to meet your individual needs as a wearer. Our medical compression stockings look good to wear, similar in style to classic fabrics and socks, but with a built in vein supporting action.
*Rabe E et al. Indications for medical compression stockings in venous and lymphatic disorders: An evidence-based consensus statement. Phlebology 2018;33(3):163-184.