- Free First Class Delivery
- Buyer Protection
- Secure Online Shopping
- Healthcare Professional? Click here
Osteoporosis


Categories
What is osteoporosis?
Osteoporosis is a metabolic disease of the skeleton where the bones lose calcium and their subsequent strength. They become porous in nature which can cause fractures – especially in the spine and femoral neck.
According to the World Health Organisation (WHO), osteoporosis is one of the most serious diseases of our time. In the EU there are more cases of osteoporosis than of breast cancer, stroke and heart attack diseases*.
The major challenge for doctors and patients is to make the diagnosis quickly. If osteoporosis is diagnosed at an early stage it can be treated effectively; however, a complete cure is not possible.
Various measures such as exercise and a healthy diet (vitamin D and calcium) also help to prevent osteoporosis.
Causes: How does osteoporosis develop?
Bones are normally viewed as rigid, solid structures that hardly change. However, a healthy skeleton is in a constant balance between the decomposition and formation of new bone. Hormones, vitamins and other messenger neurotransmitters in the body control these “remodelling measures”. Formation predominates up to approximately the age of 30. If more bone mass is broken down than is newly formed, bones lose strength and become more susceptible to fractures. This is the point where the gradual process of osteoporosis can begin.
Doctors diagnose bone loss by measuring bone density.
Osteoporosis is divided into two different forms, primary and secondary osteoporosis.
Primary osteoporosis
Approximately 95 percent of all bone loss disorders are primary osteoporosis.
Risk factors for the development of primary osteoporosis:
- Hereditary disposition
- Hormones (late first and early last menstrual period)
- Inactivity
- Long periods of bed rest
- Being underweight
- Low-calcium or high-phosphate diet (e.g. fast food, soft drinks)
- Consumption of things such as alcohol, coffee and cigarettes
Secundary osteoporosis
Secondary osteoporosis occurs as a result of certain pre-existing conditions or as an undesirable side effect of certain medication. These include:
- Anti-inflammatory drugs for the treatment of asthma or rheumatism (cortisone)
- Hormonal disorders such as hyperthyroidism
- Tumour diseases
Risk factors for the development of secondary osteoporosis:
- Anti-inflammatory drugs for the treatment of asthma or rheumatism (cortisone)
- Thyroid hormones in too high doses
- Coumarin derivatives (Marcumar)
- Chronic food intake abnormalities, e.g. due to diseases of the pancreas, intestines, liver and kidneys
- Hormone disorders, such as hyperthyroidism or diabetes mellitus (diabetes)
- Tumour diseases
Recognising osteoporosis: Symptoms and signs
A prompt diagnosis is crucial to immediately start therapy as necessary. It is therefore advisable to have a regular check-up with your doctor and have your first symptoms checked for osteoporosis. The elderly should be aware of their body’s signals and consult a doctor if bone loss is suspected. Bone density measurement provides information about the condition of the bones. If you have these symptoms, please consult your doctor as they may indicate bone loss.
- Decrease in physical height and signs of hunchback development
- Severe, chronic pain in the area of the spine or sternum
- Bone fractures without recognisable causes, e.g., vertebral fractures caused by your own body weight
How to prevent osteoporosis
Preventive measures should also be taken by young people to minimise the risk of osteoporosis later in life. Important factors for healthy bones are:
- Exercise and moderate muscle training. Specific exercises help to strengthen the various muscle groups and limit bone loss.
- A healthy and balanced diet with sufficient vitamins, calcium, and protein.
The combination of physical activity and appropriate nutrition supports the health of bones and muscles.
Osteoporosis Therapy
Therapy with various elements can contribute to significantly improving patients’ quality of life. Osteoporosis therapy consists of various elements and should be conducted according to the guidelines.
Effective osteoporosis therapy comprises several steps:
Medication for the treatment of osteoporosis
The following medication is used to treat bone loss:
Calcium and vitamin D
Calcium and vitamin D form the basis of prevention and treatment. Calcium constitutes the largest part of the mineral bone substance. Vitamin D promotes the dietary uptake of calcium, supports the incorporation of calcium in the bones and improves muscle function.
Bisphosphonates
Bisphosphonates inhibit the cells that are responsible for breaking down bone. This slows bone breakdown and the bone mass increases, which can considerably lower the risk of further fractures of the vertebral column and limbs.
SERMs
Selective oestrogen receptor modulators (SERMs): The most common cause of osteoporosis in women is the lack of the hormone oestrogen after the menopause. In the absence of oestrogen, the breakdown of bone mass increases. However, although oestrogens can prevent the further breakdown of bone, they do, at the same time, increase the risk of breast cancer and cardiovascular diseases and are therefore not recommended for the treatment of osteoporosis. Oestrogen receptor modulators, on the other hand, act on the oestrogen binding sites in the bone, but not on those in the breast or uterus, and can thus be used for treatment.
Painkillers
Painkillers: fractures cause pain. The vertebral body fractures that often occur with osteoporosis particularly limit mobility. Therefore the pain must first be treated with appropriate drugs. Back braces support medicamentous pain control by decompressing the affected vertebral bodies.
Parathyroid hormone / teriparatide:
Parathyroid hormone / teriparatide: Stimulates the formation and activity of osteoblasts. Osteoblasts are cells that are responsible for the formation of bone tissue during bone remodelling.
Sport and exercises for osteoporosis – exercises to strengthen the muscles and promote mobility
Exercise is important in the treatment of osteoporosis. Targeted physiotherapy and physical treatments, developed in collaboration with physiotherapists and doctors, helps to strengthen the muscles and promote mobility and coordination.
Exercise therapy – especially strengthening the back and abdominal musculature – should be undertaken consistently.
Specific back orthoses with bio-feedback support the spinal column and promotes muscle strengthening. In addition to physiotherapy exercises, some sports are particularly beneficial for patients suffering from osteoporosis:
- Hiking
- Swimming
- Dancing
Outdoor exercises are especially effective as sunlight stimulates the formation of vitamin D in the skin.
Training plan for osteoporosis
The optimum approach is to combine different kinds of exercise to improve strength and endurance. Increasing your muscle mass results in a better prognosis for the strength of the bone. Discover the right exercise for you and have fun with it, ensuring that you consult your doctor before training.
Functional treatment - with back orthoses
The loss of bone and muscle mass often occurs simultaneously and are diagnosed retrospectively in the UK.
Existing fractures of the spine should therefore be treated not only with medication, but also with functional therapy. Fractures cause pain which lead to further muscle loss due to sometimes severe movement restrictions. Modern spinal supports achieve a straightening of the spine and train the muscles at the same time.
In the past, patients with fractures of the spine caused by osteoporosis were often immobilised by a rigid corset, which regrettably resulted in further muscle loss. It is now known that, in addition to medicinal treatment, muscle activity plays a crucial role in bone formation.
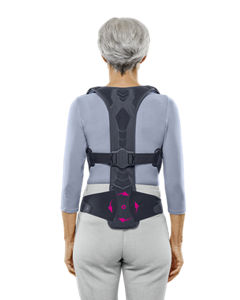
Products by medi: Osteoporosis therapy with back orthoses
Osteoporosis-related spinal fractures cause pain, further movement restrictions and often lead to progressive muscle loss. Back orthoses are modern aids to straighten the spine and to train the muscles.


It is recommended to make use of the spine-straightening orthoses **. The explicit recommendation is based on the high quality of the clinical evidence. The two studies on Spinomed and Spinomed active***,****.
- show that the back and abdominal musculature are strengthened by up to 73 and 56 percent respectively,
- a reduction of the tendency to fluctuate by up to 25 percent,
- a reduction of the kyphosis angle by up to 11 percent,
- a reduction of pain by up to 47 percent,
- improved physical comfort by up to 18 percent and
- improved pulmonary function by up to 19 percent.
The German osteoporosis specialist Professor Helmut W. Minne and medi have jointly developed the Spinomed and Spinomed active orthoses. The Spinomed orthosis is designed like a backpack. The body-variant Spinomed active can be worn inconspicuously under clothing. All Spinomed back orthoses are based on the principle of bio-feedback.
Health personnel will make the diagnosis and can prescribe compression stockings, e.g. from medi if necessary.
More information
Sources
* Epidemiologie der Osteoporose: Bone Evaluation Study, Deutsches Ärzteblatt 2013,4, 52 ff.
**DVO. Prophylaxe, Diagnostik und Therapie der Osteoporose bei postmenopausalen Frauen und bei Männern. 2017. Published on: dv-osteologie.org/osteoporose-leitlinien (last accessed 06.06.2018).
*** Pfeifer M et al. Die Wirkungen einer neu entwickelten Rückenorthese auf Körperhaltung, Rumpfmuskelkraft und Lebensqualität bei Frauen mit postmenopausaler Osteoporose. Eine randomisierte Studie. Am J Phys Med Rehabil 2004;83(3):177-186.
**** Pfeifer M et al. Die Wirkungen von zwei neu entwickelten Rückenorthesen auf Rumpfmuskelkraft, Körperhaltung und Lebensqualität bei Frauen mit postmenopausaler Osteoporose. Eine randomisierte Studie. Am J Phys Med Rehabil 2011;90(5):805-815.